Tibial valgus osteotomy
You have incipient internal osteoarthritis of the knee
You are going to undergo a tibial valgus osteotomy
You have incipient internal osteoarthritis of the knee
You are going to undergo a tibial valgus osteotomy
Tibial valgus osteotomy
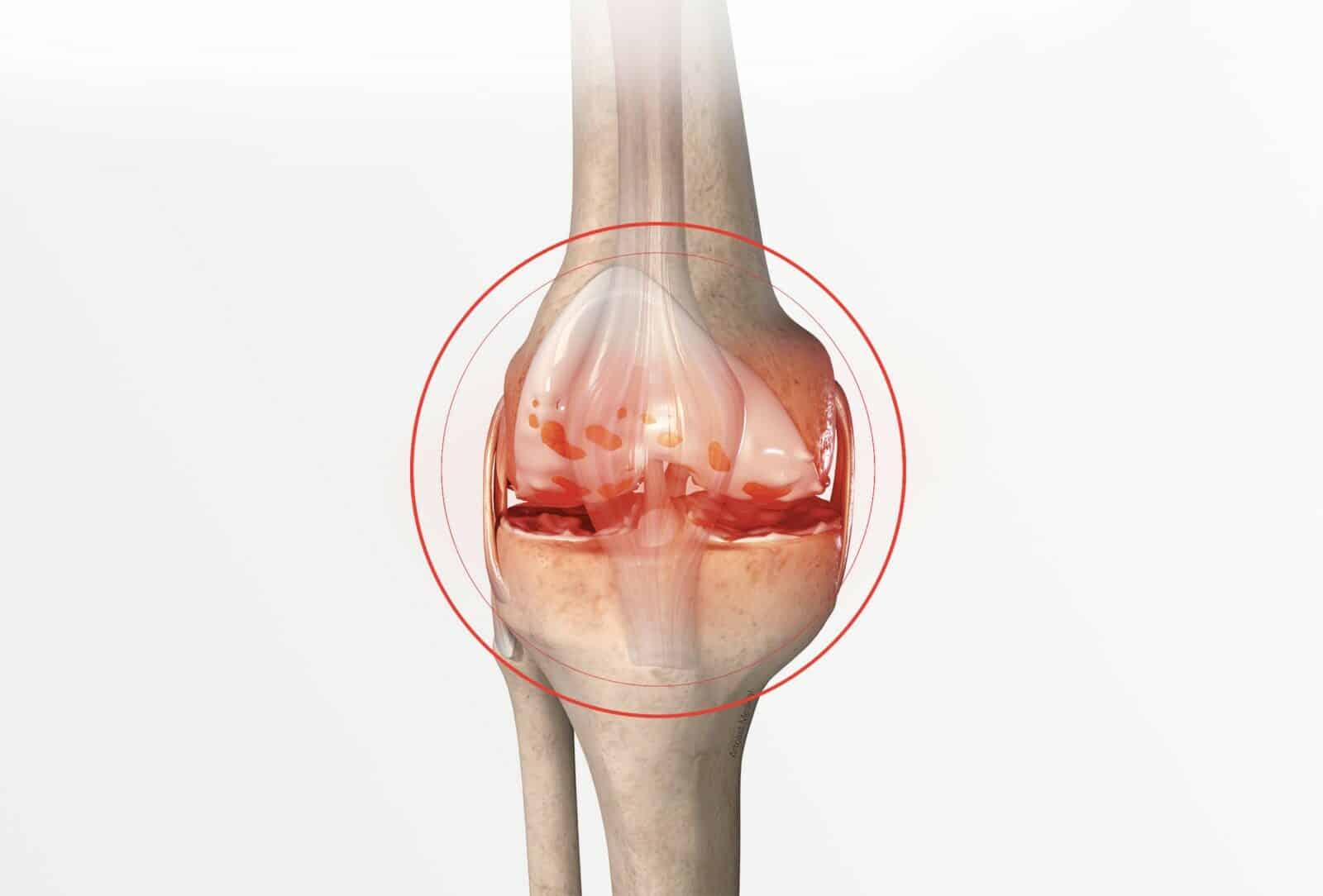
The knee is the joint between the bottom of the femur and the top of the tibia, and the sliding surfaces are lined with cartilage (figure 1). The menisci are small C-shaped cushions between the cartilage of the femur and the tibia which improve the contact and act as shock absorbers. Incipient internal osteoarthritis is the wear and tear of the cartilage between the internal part of the femur and the tibia (figure 2 and photo 1). The morphology of the lower limb is often the main cause. When curved, all the bodyweight goes through the medial part of the knee (figure 3). This overload leads to the premature wear of the cartilage and the meniscus, and causes pain in the knee as well as stiffness and difficulty in walking; it requires the use of anti-inflammatories and painkillers.

The axis of the lower limb does not correct itself spontaneously and the internal wear worsens the deformation of the limb, which in turn worsens the wear even more. The natural progression is the complete wear of the cartilage, with increased discomfort and difficulty in walking. We thus talk of advanced osteoarthritis of the knee requiring replacement. The anti-inflammatories and painkillers that were enough to start with are no longer effective, and so the question of surgery is raised. The objective of the operation is to relieve the excessive pressure on the internal part of the knee and break the vicious circle of wear in young subjects. This will relieve the pain and slow the progression of the osteoarthritis.
A tibial valgus osteotomy aims to realign the axis of the lower limb. This realignment is achieved by partially cutting and opening the top of the tibia just below the knee joint. A short incision is made in the lower internal part of the knee. The tibia is exposed and the tendons, arteries and nerves are moved aside. A pin visualising the future bone cut is placed under x-ray control.

The tibia is then partially cut with a saw, leaving an external part intact which will act as a bone hinge (figure 4). The realignment of the axis of the limb is achieved by opening up the cut, exploiting the elasticity of the external hinge (figure 5). The size of the opening is calculated according to the initial deformation and controlled by a perioperative x-ray. A plate is then fixed with screws to maintain the correction. A bone substitute is placed in the opening to fill the space and promote bone healing. A bone graft taken from the pelvis is preferred in some cases (figures 6 and 7, photo 2).
An arthroscopic knee lavage can also be carried out to rectify meniscal or cartilage damage. The operation lasts about 1 hour on average and requires around 5 days in hospital. A tibial valgus osteotomy can be performed under spinal or general anaesthesia. Your anaesthesiologist will decide with you the best type of anaesthesia according to your state of health. After the operation, the incisions are covered with a sterile dressing, which is left in place for 15 days. The pain will be managed and monitored very closely during the post-operative period, and the treatment will be adjusted accordingly. A brace will be used to immobilize and protect your knee.
During the first 6 weeks post-op, you will have crutches to help you move around so as not to put too much weight on the knee. During this period a brace is worn when moving around and at night. The rehabilitation is generally carried out by your physiotherapist. The objective is firstly to reduce the initial pain and maintain flexibility and mobility, then to recover muscle strength and sensations in the knee. Except for very specific cases, it is not necessary to go to a rehabilitation centre. Driving can be envisaged after the 2nd month, and you can generally return to work after the 3rd month, depending on your profession; office work can be sooner. A progressive return to sports activities can be envisaged after the 6th month.
In addition to the risks associated with any surgery and the anaesthetic, there are some risks specific to this surgery :
This list of risks is not exhaustive. Your surgeon can provide you with any additional explanations and will be available to discuss the advantages, disadvantages and risks of each specific case with you.
The results of this technique are well known as the procedure is over 40 years old. In more than 90 % of cases the pain disappears and mobility and muscle strength are recovered. Normal walking with no limping is generally recovered in the 3rd month post-op. The return to activities is often unrestricted. Contrary to knee replacement, the knee remains completely natural and all types of sports activities are possible. Nevertheless, certain demanding activities such as running can promote the deterioration of the cartilage and comprise the long-term result. The beneficial effect of a tibial valgus osteotomy is approximately twelve years, thus delaying knee replacement by as many years.
Laissez votre commentaire