Calcific tendonitis of the shoulder
You have calcific tendonitis of the shoulder
You are going to undergo an arthroscopic debridement of calcific tendonitis

You have calcific tendonitis of the shoulder
You are going to undergo an arthroscopic debridement of calcific tendonitis
Calcific tendonitis of the shoulder
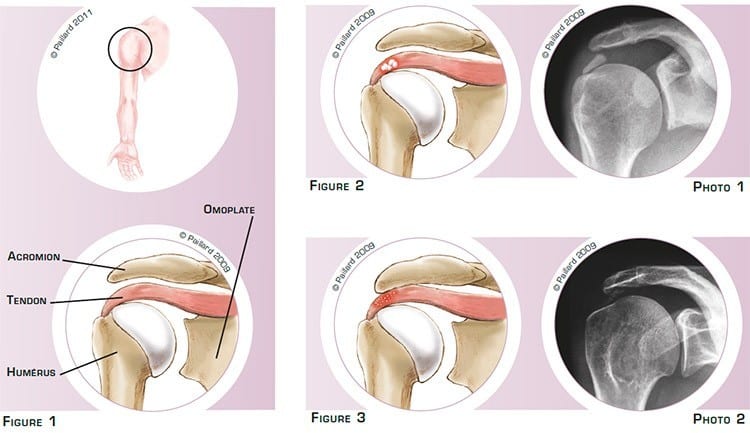
The shoulder is the joint between the scapula and the humerus. The superior part of the humerus comprises a head that pivots in the glenoid cavity of the scapula. The acromion is part of the scapula, which forms an arch above the joint. The tendons connecting the muscles to the bone are attached to the head of the humerus and slide between the head and the acromion during lifting of the arm and rotation of the shoulder (figure 1).
Calcific tendonitis is the accumulation of calcium deposits on one or several tendons.
The deposits can be isolated, resembling chalk dust or toothpaste, and can result in an inflammation of the tendons (figure 2 and photo 1).
In other cases, the deposits can be more diffuse within the tendon. It is often associated with a thick, aggressive acromion, which sometimes forms a bone spur and irritates the tendon (figure 3 and photo 2).
Calcific tendonitis causes pain and even a decrease in shoulder mobility requiring the heavy use of oral painkillers and anti-inflammatories or injections as well as physiotherapy.
The calcific deposits can disappear spontaneously over several months or years. However, the absence of any positive natural progression and in the face of persistent pain, even with medical treatment and physiotherapy, raises the question of the need for surgery. The objective of the operation is to relieve the pain, recover joint mobility and normal use of the arm.
Calcific shoulder tendonitis is treated arthroscopically, that is, without opening the joint. Arthroscopy spares the anatomical structure and the joint can be accessed without damaging the muscles. This technique therefore has proven advantages in relation to traditional surgery, including minimal blood loss and faster post-operative recovery.
Two or three small 5mm incisions are made around the shoulder. An arthroscope, or small camera, is inserted through one of the incisions to view the joint and in particular the tendons. Small instruments are inserted through the other incisions to perform the surgery.
If the deposits are discrete, a simple debridement is carried out :
After cleaning the shoulder and resecting the inflamed tissue, the exact location of the calcific deposit is marked precisely using a needle.
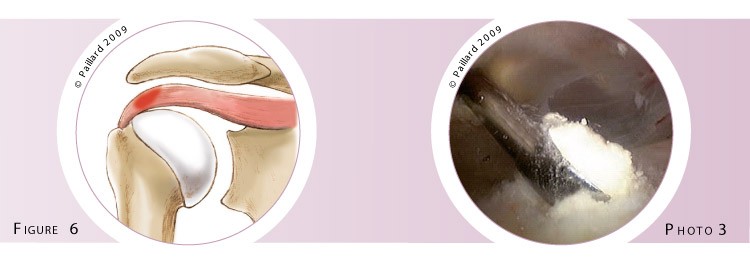
The tendon is then cut as little as possible along the length of the fibre to enable good healing after the operation (figure 4). The calcific deposit is then removed using a curette or a motorised instrument that destroys and sucks up the calcific deposit at the same time (figures 5 and 6, photo 3).

In the case of diffuse calcific deposits, partial excision is combined with an acromioplasty :
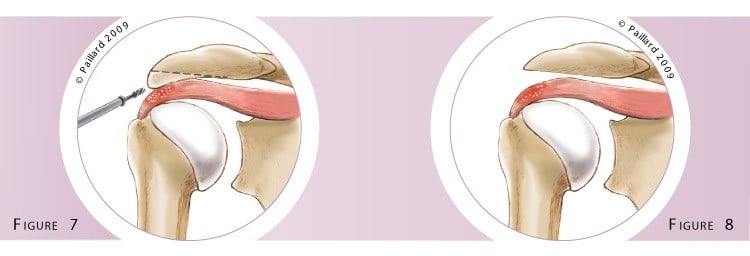
The acromion bone is freed and clearly exposed. The aggressive part of the acromion is marked then resected using a motorised cutter that cuts the bone and sucks up the debris (figure 7). The acromion is therefore progressively thinned and the bone spur completely removed. At the end of the operation, we check that it is completely flat and that it no longer irritates the tendons during movement (figure 8).
The operation lasts about half an hour on average, and requires about 2 days in hospital.
The operation is carried out under regional or general anaesthesia. Your anaesthesiologist will decide with you the best type of anaesthesia according to your state of health.
After the operation, the incisions are covered with a sterile dressing, which is left in place for 10 days. The pain will be managed and monitored very closely during the post-operative period, and the treatment will be adjusted accordingly. You will wear a brace to immobilize and protect your shoulder.
The day after the operation, the physiotherapist will help you move your shoulder. You will abandon the brace within a few days. The rehabilitation, which consists in recovering shoulder flexibility and coordination, will take place at your physiotherapist’s.
Driving can be envisaged after about 15 days, and you can generally return to work during the 2nd month, depending on your profession; office work can be sooner.
A return to sports activities that do not put any strain on the shoulder can be envisaged during the 2nd month. You will have to wait until 4 months post-op before a full return to sports, particularly those that put strain on the shoulder.
In addition to the risks associated with any surgery and the anaesthetic, there are some risks specific to this surgery :
This list of risks is not exhaustive. Your surgeon can provide you with any additional explanations and will be available to discuss the advantages, disadvantages and risks of the operation with you.
For discrete forms, complete recovery generally takes about 3 to 6 months. The end result depends on the extent of the excision. It is judged satisfactory in over 90 % of cases.
For diffuse forms, complete excision is more difficult and the calcific deposits disappear progressively over time. Recovery can therefore take a little longer.
The results of this surgery are however very encouraging as a disappearance of the pain is observed in over 85 % of cases and satisfactory function is recovered in over 95 % of cases.
These results are maintained over time as a rupture of the tendon is observed in less than 5 % of cases and the risk of relapse is virtually zero.
Laissez votre commentaire